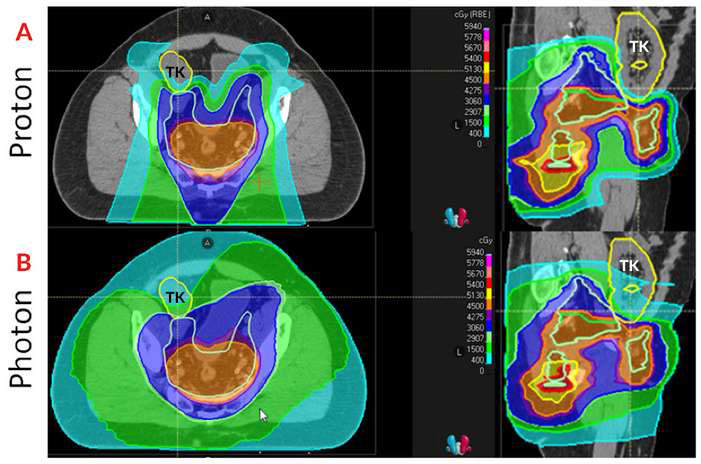
Proton Therapy Case Study: Gastrointestinal Oncology
Diagnosis: Recurrent anal squamous cell carcinoma in a patient with a pelvic kidney
Presentation and Examination
The patient is a 48-year-old male who underwent an orthotopic kidney transplant 20 years ago and was subsequently diagnosed with an anal squamous cell carcinoma (SCC) in 2009. At the time of the original diagnosis, he was treated with a surgical excision followed by pelvic radiotherapy. He recently presented with a new anal mass.
A pelvic MRI identified a 3.7 cm mass at the anal verge. The following month, staging CT scans of the chest and abdomen were negative for other sites of disease. An excisional biopsy of the mass revealed SCC. A subsequent staging PET/CT scan identified a 3.8 cm tumor with a standard uptake value (SUV) of 4.6. There was no lymph node involvement, and no metastasis was found.
Treatment Plan
The patient’s diagnosis was discussed at the Inova Schar Cancer Institute’s Multidisciplinary Gastrointestinal Oncology Tumor Board. Surgical options included a salvage abdominoperineal resection, requiring a permanent colostomy after surgery. The patient desired a nonsurgical treatment option and considered palliative (noncurative) chemotherapy. After further discussion, reirradiation utilizing proton therapy was considered. Proton therapy was determined to be the best option to treat the tumor, since it would protect the patient’s transplanted kidney while still allowing for safe reirradiation to a curative dose.